|
|
|
Indian Pediatr 2016;53: 352 |
 |
Neonatal Melioidosis with Pneumatoceles
|
|
*S Nivedhana and Shobana Rajendran
CHILDS Trust Medical Research Foundation, Kanchi
Kamakoti CHILDS Trust Hospital, Chennai,Tamil Nadu, India.
Email: *[email protected]
|
|
Melioidosis is a glanders like infectious disease caused by
Burkholderia pseudomallei, a soil saprophyte which is endemic in
tropical countries [1]. We report meliodosis in a late preterm (36 weeks
born by Caesarian section, for fetal distress) male neonate (birth
weight 4 kg). The antenatal history was unremarkable; spontaneous
rupture of membranes occurred pramaturely. The Apgar scores were 7 and 8
at 1 and 5 min, respectively. The neonate was hypoxic at birth and was
administered oxygen for 2 days in the neonatal intensive care unit
(NICU). He improved on day 3 and was started on direct breast feeding.
On day 5, the neonate had fever and tachypnea for
which he was shifted to NICU and started on oxygen and antibiotics (Ampicillin
and Amikacin). On day 6, respiratory distress worsened, and he developed
septic shock for which he was mechanically ventilated and given
inotropes and platelet infusion. Antibiotics were upgraded to Meropenem
and Vancomycin.
 |
|
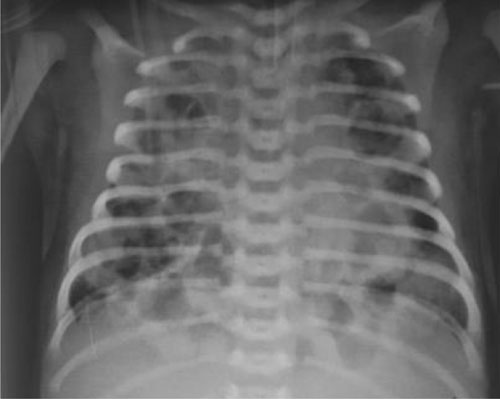
Fig. 1 Chest X-ray showing extensive
bilateral pneumatoceles.
|
He was shifted to our neonatal unit on day 8, with
signs of shock in the form of central cyanosis, hypotension and absent
peripheral pulses. There was abdominal distension with
hepatosplenomegaly. Investigations revealed leukopenia (total leukocyte
count 3100 cells/mm 3, P-14%,
L-84%, M-2%) with severe thrombocytopenia (platelet count 25,000
cells/mm3), raised
C-reactive protein (194 mg/L), hypocalcemia and mixed acidosis. Chest
X-ray showed diffuse bilateral pneumatoceles, and echocardiography
documented severe pulmonary hypertension. He was managed with high
frequency ventilation, inhaled nitric oxide, inotropes and steroids.
With worsening hypoxia and acidosis, he died within 8 hours of
admission. Blood culture (BacT/ALERT PF plus medium) grew B.
Pseudomallei, identified using Vitek-2 (Biomerieux, France).
Common presentations of neonatal melioidosis are
fever, respiratory distress, bacteremia and meningitis. The mortality in
neonatal melioidosis is high as compared to pediatric melioidosis.
Ceftazidime is the drug of choice; meropenem is an alternative.
Treatment with aminoglycosides, ciprofloxacin and colistin results in
treatment failure [2].
This neonate’s mother was an agricultural worker and
could have contracted the infection from contact with water or soil [3].
There are less chances of infection being nosocomial, as the neonate was
symptomatic at birth. Blood culture was not taken from the mother, and
hence a rare possibility of transplacental spread or spread via breast
milk could not be excluded [4,5]. Our report alerts both the clinicians
and microbiologists about the rare occurence of melioidosis in febrile
children and neonates from rural background, who are admitted with
severe respiratory distress.
References
1. Dias M, Antony B, Aithala S, Hanumanthappa
B, Pinto H, Rekha B. Burkholderia pseudomallei septicaemia - A
case report. Indian J Med Microbiol. 2004;22:266-8.
2. Lumbiganon P, Pengsaa K, Puapermpoonsiri S,
Puapairoj A. Neonatal melioidosis: A report of 5 cases. Pediatr Infect
Dis J. 1988;7:634-6.
3. Noyal MJ, Harish BN, Bhat V, Parija SC. Neonatal
melioidosis: A case report from India. Indian J Med Microbiol. 2009;27:260-3.
4. Abbink FC, Orendi JM, de Beaufort AJ.
Mother-to-child transmission of Burkholderia pseudomallei. N Engl
J Med. 2001;344:1171-2.
5. Ralph A, McBride J, Currie BJ. Transmission of
Burkholderia pseudomallei via breast milk in Northern Australia.
Pediatr Infect Dis J. 2004;23:1169-71.
|
|
|
 |
|

