An 11-year-old boy presented with slightly itchy skin eruption on his
palms for the preceding 5 days. Examination revealed multiple circular
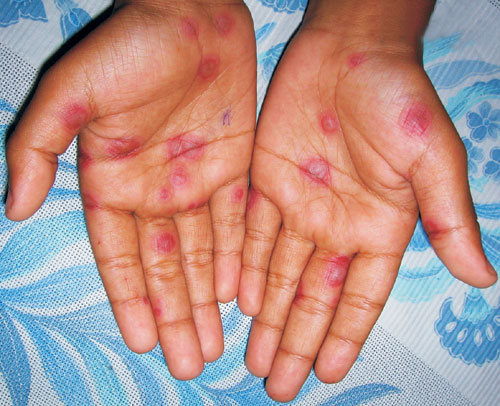
plaques with central dusky coloration, bullae formation, and peripheral
erythematous rings on his palms. The central bullae or dusky coloration
with surrounding concentric rings resemble the appearance of a ‘target’. A
few similar skin lesions were also seen on the other areas of his body.
There was no mucosal lesion. Based on the distinctive clinical feature, a
diagnosis of Herpes simplex-associated erythema multiforme (EM) was made (Fig.
1).
 |
|
Fig.1 Erythema multiforme |
Erythema multiforme is a cutaneous reaction pattern
precipitated mainly by various infections and drugs. Herpes simplex virus
(HSV) 1 and 2, adenovirus, measles, Mycoplasma, and Yersinia
are considered important infectious cause of EM amongst others. Drugs like
sulfonamides, penicillin, cephalosporin, and tetracycline may also
precipitate EM. Rare causes of EM include malignancies and collagen
vascular diseases. However, no underlying cause is found in a number of
cases.
Other differential diagnoses that should be considered
in the present case are: urticaria, hand foot and mouth disease (HFMD),
fixed drug eruption (FDE), vasculitis, and urticarial vasculitis. In
urticaria the central zone comprises of normal skin, lesions usually
change within hours, associated with swelling, and lesions resolve and
re-appear at different sites on daily basis. On the other hand, the
central zone of EM is damaged skin, lesions are symmetrical, fixed (at
least for some days), and all lesions usually appear within a few days.
FDE may resemble EM, but usually the lesions are solitary or a few
compared with multiple lesions of EM. FDE usually manifests as round or
oval, sharply delineated erythematous plaque the center of which may
blister or become necrotic. It gradually fades away with residual
hyperpigmentation. Moreover, recurrent lesions usually appear at the same
anatomical site. In HFMD, the characteristic rash consist of flat or
raised erythematous lesions, sometimes with vesicles with a perilesional
erythematous halo and are usually located on the palms, soles, knees and
buttocks. The lesions on the palms and soles are characteristically
elliptical in shape. Associated buccal mucosal lesions are usually
present. Vasculitis or urticarial vasculitis may also mimic EM, but the
target lesions are usually absent. Finally, histopathological examination
of the lesional skin often helps to differentiate EM from other close
mimickers.
EM is usually a self-limiting condition and management
should focus on treating the underlying infection or immediate withdrawal
of the offending drug. Oral acyclovir has been shown to be beneficial in
EM caused by HSV and also in suppression of recurrent EM.

