|
|
|
Indian Pediatr 2013;50: 1047-1050 |
 |
Survival and Morbidity Among Two Cohorts of
Extremely Low Birth Weight Neonates from a Tertiary Hospital in
Northern India
|
|
Kanya Mukhopadhyay, Deepak Louis, Srinivas Murki, Rama Mahajan, *MR
Dogra and Praveen Kumar
From the Neonatal Unit, Department of Pediatrics; and
*Department of Ophthalmology; Postgraduate Institute of Medical
Education and Research, Chandigarh, India.
Correspondence to: Dr Kanya Mukhopadhyay,
Additional Professor, Department of Pediatrics, PGIMER,
Chandigarh 160 012, India.
Email: [email protected]
Received: December 12, 2012;
Initial review: January 24, 2013;
Accepted: May 14, 2013 ;
Published online: June 5, 2013.
PII: S097475591201081
|
This study was conducted to
compare the survival and morbidity of extremely low birth weight
neonates born during two different time periods (2009-10 and
2001-02) at a Level III referral neonatal unit in Northern India.
All consecutive intramural extremely low birth weight neonates
(<1000g), irrespective of gestation, and admitted to Intensive Care
were enrolled. 149 and 123 neonates were enrolled during 2009-10 and
2001-02, respectively. The baseline characteristics were comparable
except for mean birth weight, which was lower during 2009-10
(843±108g vs 885±126g, P=0.003). Surfactant therapy
(54% vs 18%, P<0.001), non-invasive ventilation (28%
vs 6%, P<0.001), high frequency ventilation (24% vs
4%, P=0.001), IVH (52% vs 25%, P<0.001) and PDA
(34% vs 18%, P=0.004) were significantly more during
2009-10. Culture positive sepsis (33% vs 51%, P=0.003)
and ROP rates (7% vs 23%, P=0.042) were significantly
higher during 2001-02. Overall survival was similar; however,
neonates between 28-30 weeks gestation had better survival (63%)
during 2009-10 compared to 2001-02 (38%), P=0.009. Survival
in neonates 28-30 weeks improved during this period while overall
survival remained the same.
Keywords: Comparison, ELBW neonate, India,
Morbidity, Outcome, Survival.
|
|
Extremely low birth weight
(ELBW) neonates (<1000g at birth) form a very special high risk cohort
among neonates, and are the most vulnerable for developing varied
morbidities. Data on survival and morbidity of ELBW neonates are mostly
from developed countries. It suggests a significant decline in mortality
among ELBW neonates between 1990-91 and 1995-96 [1]. They also found
that incidence of major disorders including necrotizing enterocolitis
(NEC), intraventricular hemorrhage (IVH) and bronchopulmonary dysplasia
(BPD) increased from 1990-91 to 1995-96 while it remained static between
1995-96 and 1997-2002.
Similar information is lacking from developing
countries [2,3]. However, there is no data showing trends in mortality
or the incidence of morbidities among ELBW neonates from our country.
Thus, we compared the survival and morbidity among ELBW neonates born in
our centre during 2009-10 and 2001-02.
Methods
This study was conducted in a level III referral
neonatal unit of a teaching hospital in Northern India. All intramural
ELBW neonates born during two separate time-periods, i.e.
2009-2010 and 2001-02 and admitted to neonatal intensive care were
enrolled. Those with major/life threatening malformations were excluded.
Extramural neonates were not included. Gestational age was based on
maternal last menstrual period, and when available, ultrasound based
assessment was used and confirmed postnatally by New Ballard Score [4].
Small for gestational age (SGA) was defined when birth weight was <10 th
centile as per Lubchenco’s intrauterine growth charts [5]. Morbidities
affecting these neonates and their mortality during hospital stay were
recorded. These neonates were followed till death or discharge from the
hospital. Informed consent was obtained from parents and the Institute
Ethics Committee approved the study.
After initial stabilization in the delivery room,
these neonates were shifted to intensive care unit with consent of
parents who were willing for care. Neonates with respiratory distress
syndrome were managed with early rescue surfactant and early continuous
positive airway pressure (CPAP) during 2009-10, while its use was less
during 2001-02 due to non-availability of surfactant. Those who failed
CPAP were given a trial of nasal intermittent positive pressure
ventilation (NIPPV) during the period 2009-10 before initiating
mechanical ventilation. High frequency ventilation was used as a rescue
mode during both time periods. Trophic feeding was initiated at the
earliest and transitioned gradually to full feeds depending on their
tolerance, which was similar during both time periods. Blood culture by
BACTEC method was used for
bacterial isolation in neonates during 2009-10 while conventional blood
cultures were used during 2001-02 period. Echocardiography was used for
identification of hemodynamically significant patent ductus arteriosus
(PDA) in symptomatic babies. Screening head ultrasonogram (USG) was done
once before day 4 of life, on day 7-14 of life and prior to discharge or
at 36 to 40 weeks postmenstrual age (PMA) in asymptomatic babies by a
trained neonatologist. Retinopathy of prematurity (ROP) screening was
done at 28 days postnatal age by trained ophthalmologists and laser
therapy provided, when indicated.
Standard definitions were used for defining various
morbidities during both time periods. BPD was defined based on the
criteria of receiving oxygen therapy of >21% for
³28 days [6]. IVH was
graded using Volpe’s classification [7]. NEC was defined as per modified
Bell’s staging [8]. ROP was classified using International
Classification of Retinopathy of Prematurity (ICROP) classification [9].
Statistical analysis: Descriptive statistics was
used for describing baseline variables. Chi-square test was used for
categorical variables and independent t test or Mann Whitney U test was
used for continuous variables depending on their distribution. A P
value of <0.05 was considered significant.
Results
During 2009-10, 149 of 255 ELBW neonates and during
2001-02, 123 of 181 ELBW neonates were shifted to NICU and enrolled (Table
I). The remaining neonates were not shifted due to either
non-availability of beds, parents unwilling for care or death in labor
room. Birth weight was significantly lower in neonates born during
2009-10 compared to 2001-02 while gestational age was similar. Antenatal
steroids was received by 111 (75%) mothers during 2009-10, while this
data was not available for 2001-02.
TABLE I Baseline Characteristics of ELBW Neonates
|
2009-10 |
2001-02
|
|
(n=149) |
(n=123) |
|
Gestational age (wks) |
29.1 ± 2.6
|
29.5 ± 2.6
|
|
Birthweight* |
843 ± 108
|
885 ± 126
|
|
Males |
78 (52) |
66 (54) |
|
SGA |
77 (52) |
57 (46) |
|
LSCS |
48 (32) |
32 (26) |
|
Maternal medical illness*
|
33 (22) |
14 (11) |
|
Obstetric complications*
|
127 (85) |
91 (74) |
|
Apgar at 1 min*# |
6 (3,7) |
6 (5,7) |
|
Apgar at 5 min*# |
8 (6,9) |
8 (7,8) |
|
Values represent mean ± SD and n (%);
#represent median [IQR]. SGA – small for gestational age; LSCS – lower segment caesarean section; *P<0.05. |
Comparison of morbidity is depicted in Table
II. Surfactant therapy, ventilation including noninvasive
ventilation and high frequency ventilation, PDA, IVH including grade 3
or 4 IVH were significantly more common during 2009-10 while culture
positive sepsis and ROP were more during 2001-02.
TABLE II Morbidity in ELBW Neonates During The Two Periods Under Study
|
2009-10 |
2001-02 |
P
|
|
(n=149) |
(n=123) |
value |
|
Respiratory distress at birth |
104 (70) |
92 (75) |
0.43 |
|
RDS |
48 (46) |
58 (63) |
|
|
Congenital pneumonia |
26 (25) |
14 (15) |
|
|
TTNB |
30 (29) |
20 (22) |
|
|
Surfactant therapy |
56 (54) |
23 (25) |
<0.001 |
|
Any ventilation during hospital stay |
99 (92) |
66 (72) |
0.02 |
|
Only non invasive ventilation |
29 (28) |
7 (8) |
<0.001 |
|
High frequency ventilation |
25 (24) |
5 (5) |
0.001 |
|
Mechanical ventilation |
67 (64) |
59 (64) |
0.79 |
|
NEC |
23(15) |
25 (20) |
0.69 |
|
NEC stage II or greater |
15 (10) |
17 (14) |
0.25 |
|
PDA |
51 (34) |
23 (18) |
0.004 |
|
Culture positive sepsis |
49 (33) |
63 (51) |
0.003 |
|
IVH any grade |
78 (52) |
32 (25) |
<0.001 |
|
IVH grade 3 or 4 |
39 (26) |
14 (11) |
0.002 |
|
BPD |
19 (13) |
9 (7) |
0.14 |
|
ROP |
10 (7) |
28 (23) |
0.042 |
|
ROP requiring laser therapy |
2 (1.3) |
10 (8) |
0.85 |
|
Values represent n (%).
NEC-necrotizing enterocolitis, PDA-patent ductus arteriosus,
IVH- intraventricular hemorrhage, BPD-bronchopulmonary
dysplasia, ROP-retinopathy of prematurity. |
Seventy-eight neonates (52%) survived during 2009-10
period while 56 (46%) survived during 2001-02. Their survival comparison
is depicted in Table III. None of the neonates <500g
during either time periods survived. Overall survival rate was similar
in 2 periods but survival at 28-30 weeks gestation improved
significantly (P=0.009) from 38% in 2001-2 to 63% in 2009-10.
TABLE III Survival Based on Gestational Age and Birth Weight during both Time Periods
| |
Unadjusted survival |
Adjusted survival* |
|
2009-10 |
2001-02 |
P value |
2009-10 |
2001-02 |
P value
|
|
(n=255) |
(n=181) |
(n=149) |
(n=123) |
|
|
|
<28 weeks |
9/108 (8) |
10/61 (16) |
0.18 |
9/42 (21) |
10/31 (32) |
0.29 |
|
28-30 weeks |
39/95 (41) |
19/70 (27) |
0.09 |
39/62 (63) |
19/50 (38) |
0.009 |
|
>30 weeks |
30/52 (58) |
27/50 (54) |
0.86 |
30/45 (67) |
27/42 (64) |
0.82 |
|
<500g |
0/3 (0) |
0/1 (0) |
– |
0/3 (0) |
0/1 (0) |
– |
|
500-750g |
7/69 (10) |
7/48 (15) |
0.66 |
7/22 (32) |
7/21 (33) |
0.92 |
|
>750g |
71/183 (39) |
49/132 (37) |
0.86 |
71/124 (57) |
49/101 (48) |
0.19 |
|
Values are n (%). A P value <0.05 is
significant. *Adjusted included only those neonates who got
transferred to intensive care. |
 |
|
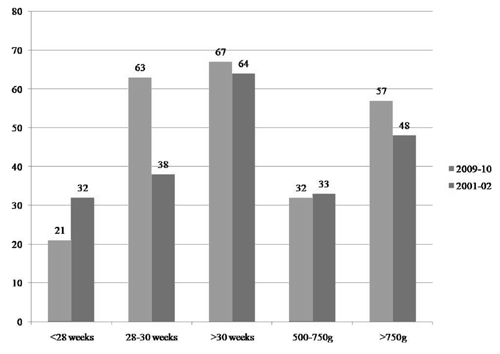
Fig. 1 Adjusted survival based on
gestation and birth weight categories during both time periods
(values represent %).
|
Discussion
The survival in 28-30 weeks gestation improved
significantly in 2009-10 probably due to surfactant therapy, and
non-invasive and high frequency ventilation. Surfactant was introduced
only in the early 2000 to India and this could explain its reduced use
in neonates born during 2001-02 compared to the later period. The
benefits of early surfactant have been clearly shown by numerous
randomized controlled trials and in a recent Cochrane review [10]. The
same reason explains the use of non-invasive ventilation, especially
CPAP, which has become a standard of care among pre-term neonates with
respiratory distress syndrome. The evidence for this comes from trials
that showed that a significant proportion of these neonates, including
the extremely low birth weight neonates, could be managed with CPAP
alone, without needing mechanical ventilation [11,12].
IVH occurred more frequently in the 2009-10 than
2001-02. IVH is multi-factorial in etiology and in our study population,
at least two of these risk factors namely PDA and mechanical ventilation
[13] were more prevalent in the 2009-10 cohort, and there were more
number of survivors in 28-30 weeks gestation who are more likely to
develop IVH. It might also be due to our increasing expertise with
neonatal imaging, especially head ultrasound and echocardiography, that
we were able to pick up more IVH and PDA during the latter period. The
decline in culture positive sepsis could be due to improvements in hand
hygiene and better aseptic precautions during procedures. This also
could be due to increased pre-treatment of mothers with antibiotics,
especially when presenting with preterm rupture of membranes in the
setting of preterm labor. Further, this occurred despite the fact that
we were using BACTEC cultures for bacterial isolation during the latter
period, which has higher rates of bacterial isolation than the
conventional cultures [13]. Lower rates of ROP could be due to more
rigorous monitoring of saturation as we became more aware of the harmful
effects of oxygen in the pathogenesis of various diseases including BPD
and ROP [14,15].
Better survival for neonates born between 28-30 weeks
during 2009-10 could be due to the advances in perinatal and neonatal
care that occurred between the two time periods, including antenatal
steroids, surfactant therapy and noninvasive ventilation. However, such
improvements were not reflected in those born <28 weeks or >30 weeks and
the reason for this is probably that we need to improve care in the <28
weeks group and the existing care is optimal at >30 weeks of gestation
though we should try to improve further. Our birth weight-wise survival
analysis did not find any significant difference between the two
periods. Fanaroff, et al. [1] from the NICHD network found that
in neonates weighing 501-750 g, mortality decreased from 59% in 1991-92
to 46% in 1995-96 and stayed at 45% for 1997-2002. For the 751-1000
category, it declined from 19% to 14% during 1991-92 to 1995-96 and it
reached 12% during 1997-2002. In a Swedish national prospective study
conducted during the years 1990-1992, the average neonatal mortality
among ELBW cohort was 37%, but their gestational ages were much lower
compared to our cohort [16]. Another retrospective study in 1998 from
Taiwan showed an overall neonatal survival of ELBW neonates to be 74%
and survival to discharge of 60% [17]. Survival was 40% for neonates
<750g and 68% for those >750g. Their survival in babies <26 weeks
gestation was 27% while those above 26 weeks, it was 72%.
The shortcomings of our study were that we did not
use an objective score to assess the severity of neonatal illness, which
could have improved the comparability between the two cohorts; and did
not systematically look at the practices that would have changed the
outcome in these neonates during these two time periods. We were also
not able to look at the effect of antenatal steroids as we did not have
data for the same in the former cohort. Optimum care could not be
provided to all ELBW neonates due to financial constraints and
non-availability of beds. The strengths are that we had adequate number
of babies who were enrolled and no previous study from India has made
such a comparison between two time periods over a period of 10 years.
In conclusion, though the survival is increasing in
our set-up, it is far below than that off from developed countries.
Contributions: KM: conceptualized the study,
supervised data collection and reviewed the manuscript; DL: Analyzed
data and prepared the manuscript; SM: Collected the data of 1st cohort;
RM: Collected the data of 2nd cohort; MR: Provided data on ROP; and PK:
Critically reviewed the manuscript.
Funding: PGI research scheme; Competing
interests: None stated.
|
What This Study Adds?
•
The Survival was found to be
improving in the last decade amongst ELBW neonates, especially
in 28-30 weeks gestation group,
|
References
1. Fanaroff AA, Stoll BJ, Wright LL, Carlo WA,
Ehrenkranz RA, Stark AR, et al. Trends in neonatal morbidity and
mortality for very low birthweight infants. Am J Obstet Gynecol.
2007;196:147 e1-8.
2. Narayan S, Aggarwal R, Upadhyay A, Deorari AK,
Singh M, Paul VK. Survival and morbidity in extremely low birth weight
(ELBW) infants. Indian Pediatr. 2003;40:130-5.
3. Sehgal A, Telang S, Passah SM, Jyothi MC. Maternal
and neonatal profile and immediate outcome in ELBW babies. Indian
Pediatr. 2003;40:991-5.
4. Ballard JL, Khoury JC, Wedig K, Wang L,
Eilers-Walsman BL, Lipp R. New Ballard Score, expanded to include
extremely premature infants. J Pediatr. 1991;119:417-23.
5. Lubchenco LO, Hansman C, Dressler M, Boyd E.
Intrauterine growth as estimated from liveborn birth-weight data at 24
to 42 weeks of gestation. Pediatrics. 1963;32:793-800.
6. Jobe AH, Bancalari E. Bronchopulmonary dysplasia.
Am J Respir Crit Care Med. 2001;163:1723-9.
7. Volpe JJ. Intraventricular hemorrhage and brain
injury in the premature infant. Neuropathology and pathogenesis. Clin
Perinatol. 1989;16:361-86.
8. Walsh MC, Kliegman RM. Necrotizing enterocolitis:
treatment based on staging criteria. Pediatr Clin North Am.
1986;33:179-201.
9. The International Classification of Retinopathy of
Prematurity revisited. Arch Ophthalmol. 2005;123:991-9.
10. Rojas-Reyes MX, Morley CJ, Soll R. Prophylactic
versus selective use of surfactant in preventing morbidity and mortality
in preterm infants. Cochrane Database Syst Rev. 2012;3:CD000510.
11. Morley CJ, Davis PG, Doyle LW, Brion LP, Hascoet
JM, Carlin JB. Nasal CPAP or intubation at birth for very preterm
infants. N Engl J Med. 2008;358:700-8.
12. Finer NN, Carlo WA, Walsh MC, Rich W, Gantz MG,
Laptook AR, et al. Early CPAP versus surfactant in extre-mely
preterm infants. N Engl J Med. 2010;362:1970-9.
13. Cetin ES, Kaya S, Demirci M, Aridogan BC.
Comparison of the BACTEC blood culture system versus conventional
methods for culture of normally sterile body fluids. Adv Ther.
2007;24:1271-7.
14. Saugstad OD. Bronchopulmonary dysplasia and
oxidative stress: are we closer to an understanding of the patho-genesis
of BPD? Acta Paediatr. 1997;86:1277-82.
15. Flynn JT, Bancalari E, Snyder ES, Goldberg RN,
Feuer W, Cassady J, et al. A cohort study of transcutaneous
oxygen tension and the incidence and severity of retinopathy of
prematurity. N Engl J Med. 1992;326:1050-4.
16. Finnstrom O, Olausson PO, Sedin G, Serenius F,
Svenningsen N, Thiringer K, et al. The Swedish national
prospective study on extremely low birthweight (ELBW) infants.
Incidence, mortality, morbidity and survival in relation to level of
care. Acta Paediatr. 1997;86:503-11.
17. Tsao PN, Teng RJ, Wu TJ, Tang JR, Yau KI. Early
outcome of extremely low birth weight infants in Taiwan. J Formos Med
Assoc. 1998;97:471-6.
|
|
|
 |
|

