|
|
|
Indian Pediatr 2013;50: 1041-1043 |
 |
Presence of Hernia Sac in Prediction of
Postoperative Outcome in Congenital Diaphragmatic Hernia
|
|
Shasanka S Panda, Minu Bajpai and M Srinivas
From Department of Pediatric Surgery, All India
Institute of Medical Sciences, New Delhi 110 029, India.
Email:
[email protected]
Correspondence to: Dr M Bajpai, Professor of
Paediatric Surgery, All India Institute of Medical Sciences, New Delhi
110 029, India. [email protected]
Received: January 01, 2013;
Initial review: February 08, 2013;
Accepted: April 26, 2013.
Published online: May 5, 2013;
PII: S097475591300004
|
|
We conducted this study to assess the
value of presence of hernia sac in prediction of postoperative outcome
in congenital diaphragmatic hernia (CDH). Data were obtained form
medical records of 70 children operated for CDH between 2002-12.
Postoperative neonatal death occurred in 1/10 (10%) of infants with a
hernia sac and 26/60 (43.3%) in cases without a hernia sac, respectively
(P =0.04). Perinatal morbidity in surviving infants was lower in
the group with a hernia sac although not significantly. We conclude that
the presence of a hernia sac is associated with better postoperative
outcome and overall prognosis of CDH.
Keywords: Congenital diaphragmatic
hernia, Hernia sac, Perinatal morbidity, Postoperative outcome.
|
|
Congenital diaphragmatic hernia (CDH) occurs in
about one out of 2000 to 5000 births with high mortality and morbidity
rates. Associations with other anomalies occur in about 10% to 50% of
cases and thereby affect the overall prognosis. The diaphragmatic defect
usually features a completely open space between the chest and abdomen,
although some infants have a membrane of parietal pleura and peritoneum
acting as a hernia sac. To find clinically relevant prognostic factors
that predict the outcome of infants with CDH has been unsuccessful. The
overall mortality rate ranges from 30% to 50% [1-3]. Many anatomic
prognostic factors like liver position, lung-to-head ratio, pulmonary
volume, location of stomach, presence of polyhydramnios, fetal pulmonary
vasculature affect the overall outcome of CDH patients [4]. We assessed
the role of the presence of a hernia sac in prediction of postoperative
outcome in CDH patients.
Methods
This study was a retrospective single-centre study
done at Department of Pediatric Surgery, All India Institute of Medical
Sciences, New Delhi, India between January 2002 and November 2012.
Medical records of all cases of CDH either born or referred to our
institute were searched. Children born alive with CDH and undergone
surgery were selected for final analysis. All newborns with chromosomal
abnormalities or other malformations were excluded from the study.
Following delivery, CDH neonates were intubated
according to their arterial blood gas parameters and respiratory
distress, and transferred to the neonatal surgical intensive care unit.
ECMO was not used in the studied population. Pulmonary artery
hypertension (PAH) was evaluated by pre and post-ductal saturation or by
echocardiography and was managed by gentle low pressure high FIO 2
ventilation, and sometimes by inhaled nitric oxide. After respiratory
and hemodynamic stabilization, surgical repair was done. Survival was
defined as discharge from the hospital. The presence of a hernia sac was
noted at the time of surgery. All the surgeries were done by a single
surgeon both in the sac and non-sac group. Morbidity in surviving
infants was defined as the length of assisted ventilation, need for
supplemental oxygen 4 weeks after surgery, need for prosthetic patch
repair, and time in neonatal surgical intensive care unit.
We analyzed our data using the Stata software version
11.0 (Stata Corp. College Station, TX). Results were calculated as
median and inter-quartile range or proportions accordingly. Medians were
compared using the Mann-Whitney test, and proportions were compared
using the Fisher’s exact test. A 2-sided P value of 0.05 or less
was considered statistically significant. Institute’s ethical committee
approval for the study was obtained.
Results
Between January 2002 and November 2012, 84 patients
with diagnosis of CDH were admitted to our NSICU either born in or
referred to our institute. Two cases with associated malformations were
excluded. Twelve patients died before surgery. Surgery was performed in
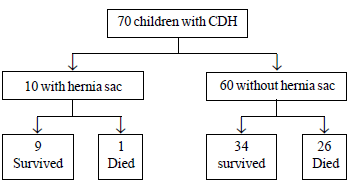
70 cases. Outcome of CDH patients according to presence of hernia sac is
depicted in Fig. 1. Median gestational age at birth
was 37 weeks (range 34-40) and median birth weight was 3010 grams (range
1500-4120). There were 40 male babies (57.1%). The relationship between
outcome, especially neonatal morbidity in surviving infants and the
presence of a hernia sac is presented in Table I.
 |
|
Fig. 1 Outcome of Congenital
diaphragmatic hernia (CDH).
|
TABLE I Morbidity and Outcome in CDH Patients According to The Presence/absence of Hernia Sac
|
Patient
|
Diaphrag- |
Diaphrag- |
P
|
|
characteristics
|
matic Hernia
|
matic Hernia
|
value
|
|
with sac |
without sac
|
|
|
Total n = 60 |
10
|
60
|
|
|
Survival* |
9 (90)
|
34 (56.6)
|
0.04#
|
|
PAH * |
3 (30)
|
37 (61.6) |
0.06
|
|
Right side*
|
0 (0)
|
5 (9.6)
|
-
|
|
Intrathoracic liver*
|
2 (20)
|
14 (23.3)
|
0.81
|
|
Intrathoracic stomach*
|
3 (30)
|
32 (53.3)
|
0.17
|
|
Need for patch repair* |
0 (0)
|
6 (10)
|
-
|
|
Need for supplemental
|
0 (0)
|
9 (15)
|
-
|
|
O2 after 4 weeks days* |
|
|
|
|
Duration of hospita-
|
9 (6-15)
|
15 (9-34)
|
0.12 |
|
lization$ (days)
|
|
|
|
|
Duration of assisted ventilation$ (days) |
3 (2-8)
|
6 (4-11) |
0.24 |
|
*Data is represented as n (%); $Data
is represented as median; #P value
is significant (≤0.05);
PAH, pulmonary artery hypertension; O2, oxygen. CDH: congenital
diaphragmatic hernia. |
Discussion
The present study showed that the presence of a
hernia sac significantly improves the prognosis in CDH. Hernia sac is
formed of parietal peritoneum and lung pleura and has been reported in
approximately 20% of cases [5]. In our study it was 14.3%. Only few
studies have addressed the impact of hernia sacs, and mostly in cases
with a late postnatal diagnosis of CDH [6,7]. In such cases of late
presentation of CDH, a hernia sac is found in about 35% [6,7]. Sac
prevents the upward movement of the abdominal organs and decreases the
risk of compression of the lungs and thereby there is lesser risk and
degree of pulmonary hypoplasia. The rate of herniation of liver and
stomach was not significantly different in the two groups in our study
suggesting the mechanism to be more complex. CDH originates from the
failure of closure of the pleuroperitoneal canal resulting in a complete
defect without peritoneum, pleura or muscle. A hernia sac may result
from a timely closure of the pleuroperitoneal canal without the
appropriate subsequent muscularization of the defect. Therefore, the
presence of a hernia sac could be the visible evidence of a late
herniation during the embryological period [8]. The timing of the defect
had more impact on prognosis rather than the contents of the hernia.
In a recent study by Spaggiari, et al. [9],
patients with a hernia sac had a significantly higher pulmonary volume
on prenatal magnetic resonance imaging (51.9% vs 39.3%, P=0.01).
In their study, neonatal death, either preoperative or postoperative,
occurred in 5.6% of infants with a hernia sac and 32.7% in cases without
a hernia sac, respectively (P =0.03). Neonatal morbidity in
surviving infants was lower in the group with a hernia sac although not
significantly [9].
Contributors: All the authors have contributed,
designed and approved the study; MB: will act as guarantor of the study.
Funding: None; Competing interests: None
stated.
|
What This Study Adds
• Presence of a hernia sac in congenital diaphragmatic hernia
is associated with a better post-operative outcome.
|
References
1. Beresford MW, Shaw NJ. Outcome of congenital
diaphragmatic hernia. Pediatr Pulmonol. 2000;30:249-56.
2. Mah VK, Zamakhshary M, Mah DY, Cameron B, Bass J,
Bohn D, et al. Absolute vs relative improvements in congenital
diaphragmatic hernia survival: what happened to "hidden mortality". J
Pediatr Surg. 2009;44:877-82.
3. Brownlee EM, Howatson AG, Davis CF. The hidden
mortality of congenital diaphragmatic hernia: a 20-year review. J
Pediatr Surg. 2009;44:317-20.
4. Arora M, Bajpai M, Soni TR, Prasad TR. Congenital
diaphragmatic hernia. Indian J Pediatr. 2000;67:665-70.
5. Puri P. Congenital diaphragmatic hernia. Curr Prob
Surg. 1994;31:787-846.
6. Baglaj M, Dorobisz U. Late-presenting congenital
diaphragmatic hernia in children: a literature review. Pediatr Radiol.
2005;35:478-88.
7. Cigdem MK, Onen A, Otcu S, Okur H. Late
presentation of bochdalek-type congenital diaphragmatic hernia in
children: a 23-year experience at a single center. Surg Today.
2007;37:642-45.
8. Skarsgad ED, Harrison MR. Congenital diaphragmatic
hernia: the surgeon’s perspective. Pediatr Rev. 1999;20:71-8.
9. Spaggiari E, Stirnemann J, Bernard JP, De Saint
Blanquat L, Beaudoin S, Ville Y. Prognostic value of a hernia sac in
congenital diaphragmatic hernia. Ultrasound Obstet Gynecol. 2012 May 17.
[Epub ahead of print].
|
|
|
 |
|

