|
|
|
Indian Pediatr 2009;46: 1009-1012 |
 |
Measles in Children Younger Than 9 Months in
Pakistan |
|
Ali Faisal Saleem, Anita Zaidi, Adnan Ahmed, Haider Warraich and Fatima
Mir
From Department of Maternal and Child Health, The Aga
Khan University Hospital, Karachi, Pakistan.
Correspondence to: Dr Ali Faisal Saleem, Stadium Road, PO
Box 3500, Karachi 74800, Pakistan.
Email: [email protected]
Manuscript received: September 2, 2008;
Initial review: October 10, 2008;
Accepted: March 12, 2009.
Published online 2009 April
15.
PII:S097475590800358-2
|
|
Abstract
Pakistan has one of the highest burden of measles and
measles-related deaths in the world. We compared the clinical course and
outcomes of measles in infants aged £9
months with those >9 month old amongst children admitted to a tertiary
care hospital. Data were collected by a retrospective chart review, and
compared between age £9 months
(Group A) and age >9 months (Group B). Severe malnutrition (P=0.039,
adjusted odds ratio=3.02), anemia (P=0.017), leukocytosis (P<0.001,
adjusted odds ratio 4.1), and conjunctivitis (P=0.021) were
higher in Group A children. All four deaths occurred in Group B.
Key words: Epidemic, Immunization, Measles, Pakistan.
|
|
M
easles is the most prevalent cause
of vaccine-preventable childhood deaths, with greatest mortality seen in
regions where access to primary health care is limited(1). Despite the
availability of an effective vaccine and a single causative serotype,
measles continues to cause approximately about one million deaths annually
among infants and children throughout the world(1-2). According to the
Expanded Program for Immunization (EPI) schedule for Pakistan; Measles
immunization is recommended at 9 months of age, which may be why mortality
is higher amongst infants younger than 9 months, who are too young to have
the vaccine(1-3). In 2004, an estimated 454,000 deaths were caused by
measles; most of these concentrated in developing countries like
Pakistan(4), with younger children being more frequently affected(5).
Mortality from measles is highest in children aged less than 12 months(6).
Pakistan Demography and Health Survey (2006-2007)
reports a country-wide coverage of 50-60% for measles immunization(7).
This reflects a possible gap in herd immunity. We compared the clinical
features and outcome of measles in infants younger than 9 months with
those older than 9 months to highlight the importance of age (infancy
vs. older) and vaccine status in determining clinical outcome in
children.
Methods
We retrospectively reviewed the charts of children aged
0-15 years who were discharged with the diagnosis of measles during a
period of six years (January 2001 till December 2006). We identified 225
children using coded discharge records for terms "measles", "measles with
pneumonia", and "complicated measles"; of these, 205 were included in the
final analysis. Chronically ill, immuno-compromized, and patients with any
malignancy were excluded. Information was extracted on age, gender,
weight, co-morbidity, date of admission, vaccination status, history of
exposure, laboratory parameters (hemoglobin, WBC count), length of stay,
and complications. These parameters were compared between the two groups
[(Group A, age £9
months) and (Group B, age >9 months)]. Data analysis was conducted with
SPSS 16 (version 16.0, SPSS Inc. Chicago, IL). P<0.05 was
considered significant. Variables found significant (cut off 0.25) at
univariate analysis were entered into multivariate logistic regression
analysis for calculating adjusted odds ratios (AOR). The study was
approved by the hospital ethics review committee of the Aga Khan
University Hospital, Karachi, Pakistan.
Results
The highest number of cases occurred in 2006 (68,
33.2%) and 2003 (44, 21.5%). Majority of cases were seen during the winter
and spring seasons. Males accounted for 59% of cases. Overall, 59% of
total patients were not vaccinated for measles. History of prior exposure
to measles cases was found in 8.2% cases and 29% of patients developed two
or more complications simultaneously.
Group A (£9
mo) comprised of 48 children (23.4%); of these 9 (4.4%) cases were below 6
months of age. Both groups had similar presenting complaints viz.,
fever, cough, rash, diarrhea and vomiting. A significantly greater
proportion of hospitalized measles cases below 9 months of age were anemic
(43.8%) and severely malnourished (20%), as compared to children in Group
B. There was no significant difference in the length of hospitalization
between the two groups. More than half of Group A developed pneumonia
(53%), followed by gastroenteritis (33%), conjunctivitis (23%) and
encephalitis (2%). Four patients of group B died during the
hospitalization (Table I).
Table I
Demography and Group Features
|
|
Group A |
Group B |
P value |
OR (CI) |
AOR (CI)* |
|
|
(age <9mo) |
(age >9mo) |
|
|
|
| Number of patients |
48 (23.4%) |
157 (76.6%) |
|
|
|
| Males |
29 (60.4%) |
92 (58.5%) |
0.48 |
1.10 (0. 6-2.05) |
|
| Severe malnutrition |
9 (20%) |
53 (34%) |
0.039 |
2.2 (0.9- 4.8) |
3.0 (1.2- 7.5) |
| Weight (Mean, SD) |
8.01 ± 2.5 |
16.3 ± 10.9 |
|
|
|
| History of exposure |
6 (12%) |
16 (10%) |
|
|
|
| Presenting complaint |
| Fever |
51 (100%) |
154 (100%) |
|
|
|
| Cough |
35 (67%) |
104 (68%) |
|
|
|
| Diarrhea |
20 (39%) |
49 (32%) |
|
|
|
| Vomiting |
17 (33%) |
44 (29%) |
|
|
|
| Rash |
32 (63%) |
102 (66%) |
|
|
|
| Anemia (Hb <10g/dL) |
21 (44%) |
41 (26%) |
0.017 |
0.4 (0.2- 0.9) |
0.5 (0.2 - 1.2) |
| Leukocytosis (WBC >104) |
23 (48%) |
31 (20%) |
<0.001 |
4.0 (1.9 - 8.0) |
4.1 (1.9 - 8.6) |
| Length of hospital stay mean (± SD) |
3.3 ± 2.1 |
3.6 ± 4.2 |
– |
– |
– |
|
≥ 5 days |
27 (17%) |
9 (19%) |
0.478 |
1.1 (0. 9-1.6) |
|
| Complications |
| Pneumonia |
25 (53%) |
65 (41%) |
0.128 |
1.5 (0.8- 3.0) |
1.6 (0.8- 3.4) |
| Gastroenteritis |
16 (33%) |
39 (25%) |
0.164 |
1.5 (0.7- 0.9) |
1.7 (0.7- 3.7) |
| Conjunctivitis |
11 (23%) |
63 (40%) |
0.021 |
0.4 (0.2- 0.9) |
0.4 ( 0.2- 0.1) |
| Encephalitis |
1 (2%) |
6 (4%) |
0.483 |
0.5 (0.1- 4.) |
|
| Died |
-- |
4 (2.5%) |
|
|
|
*AOR: Adjusted odds ratio. Variables that were found significant at univariate analysis level (P < 0.25) were then
taken into account for logistic regression analysis and calculating AOR.
|
Discussion
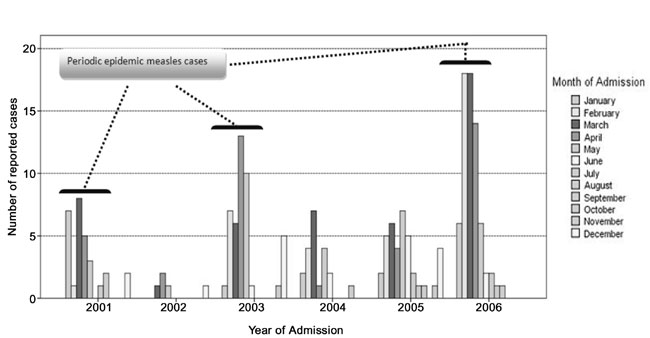
Measles is endemic to Pakistan, with periodic epidemics
occurring every 2-3 years. Figure 1 shows the
periodic epidemics and months of peak hospital admissions. The disease is
more common during the winter and spring seasons as corroborated by our
study findings. Our data showed a high incidence of measles in infants
<9months (33%) than that reported earlier (20-22% in infants aged 1 year)
from Pakistan and SEARO region (3.9% - 11.5%)(5, 8-10). This may be due to
lower levels of maternal antibody in our setting and poor baseline herd
immunity.
 |
|
|
Fig.1 Periodic measles epidemics and months of
admission. |
The vaccination status for measles in group B was low
and comparable with other Pakistani studies(5,8). Factors associated with
increased incidence of measles in regional literature are lack of or
incomplete vaccination, improper cold chain maintenance, and decreasing
immunity with age (reflects need of booster doses)(8,11-12). Our study
design and data allow us to corroborate the first and the third.
Occurrence of measles in patients with severe malnutrition is also well
reported in other studies from Pakistan with prevalence between 9 –
53%(8-12).Three of our patients died because of pneumonia, bringing the
pneumonia proportionate mortality rate to 75%, while it was 14-59% in
previous studies(8,13).
Our study reflects data from a single center, and hence
it may not be representative of the whole country. However, it does
highlight a gap in herd immunity, made evident by the increasing number of
measles patients in children <9 months. Due to the retrospective nature of
our study, we could not assess all relevant variables and had to rely on
the degree of completeness in documentation by the treating physicians. We
have however tried to reduce confounders by logistic analysis.
We propose that poor routine coverage of measles
vaccination in children >9 months and failure to catch unvaccinated
children at a later stage during a health facility visit has caused a
decrease in herd immunity in this region. This has led to periodic
epidemics, and an associated rise in morbidity in children younger than 9
months and mortality in older children. An earlier age of vaccination
should be considered in epidemic or higher endemic situations.
Acknowledgement
Dr Sabeena Jalal Khan for her help in data collection
and manuscript revision.
Contributors: AF and AZ conceptualized and
conducted the study, conducted the analysis and drafted the manuscript. AF
and FM revised the manuscript. AA and HW assisted with data analysis and
manuscript writing. All authors contributed to the manuscript preparation.
AF will act as guarantor for the paper. The final manuscript was approved
by all authors.
Funding: None.
Competing interest: None stated.
|
What this Study Adds?
• Measles is rare in younger infants where
routine immunization coverage is high, but periodic epidemics in
younger infants are seen where routine coverage is not upto the
mark.
|
References
1. Duke T, Mgone CS. Measles: not just another viral
exanthema. Lancet 2003; 361: 763-773.
2. Murray CJ, Lopez AD. Mortality by cause for eight
regions of the world: global burden of disease study. Lancet 1997; 349:
1269-1276.
3. Mgone J, Mgone C, Duke T, Frank D, Yeka W. Control
measures and the outcome of the measles epidemic of 1999 in the Eastern
Highlands Province. PNG Med J 2000; 43: 90-97.
4. World Health Organization Media Center. Measles Fact
sheet No 286 revised March 2006. www.who.int/mediacentre/factsheets/fs286/en/print.
html. Accessed 21 June, 2007
5. Tariq P. Assessment of coverage levels of single
dose measles vaccine. J Coll Phy Surg Pak 2003; 13: 507 - 510.
6. Department of Health. Measles. In: Immunisation
against infectious disease. 2005: 1-24. www.dh.gov.uk/assetRoot/04/12/44/88/04124488.pdf.
Accessed 21 June, 2007
7. National Institute of Population Studies (NIPS)
[Pakistan] and Macro International Inc. 2008. Pakistan Demographic and
Health Survey 2006-07. Islamabad, Pakistan: National Institute of
Population Studies and Macro International Inc; 2008.
8. Aurangzeb B, Nisar YB, Hazir T, Burki T, Hassan M.
Clinical outcome in children hospitalized with complicated measles. J Coll
Phys Surg Pak 2005; 15: 547-551.
9. Sharma MK, Bhatia V, Swami HM. Outbreak of measles
amongst vaccinated children in a slum of Chandigarh. Indian J Med Sci
2004; 58: 47-53.
10. Satpathy SK, Chakraborty AK. Epidemiological study
of measles in Singur, West Bengal. J Comm Dis 1990; 22: 23-26.
11. Sharma BS, Kaushik VK, Johri S. An epidemiological
investigation of measles outbreak in Alwar, Rajasthan. J Comm Dis 1984;
16: 299-303.
12. Khan HI, Ahmad TJ. Risk factors for increased
mortalilty in children with complications of measles. J Coll Phys Surg Pak
1999; 9: 247-250.
13. Duke T, Poka H, Dale F, Micheal A, Mgone J, Wal T.
Chloramphenical versus benzylpenicillin and gentamycin for the treatment
of severe pneumonia in children in Papua New Guinea: a randomised trial.
Lancet 2002; 359: 474-480.
|
|
|
 |
|

