Shaken baby syndrome (SBS) is a serious form of child
abuse which may be frequently under diagnosed because there may be no
obvious external evidence of injury(1). A review of previously reported
cases yielded only one isolated report from the Indian Sub-continent(2).
We present a child admitted with serious unexplained neurological
symptoms in whom the diagnosis was made after excluding systemic
disorders.
Case Report
This 5-month-old thriving infant was brought in a
critically unstable condition to our hospital with a history of low
grade fever for 2 days, drowsiness and recurrent seizures since the day
of admission, On arrival the baby was minimally responsive to pain and
had decerebrate posturing with bilateral sluggishly reacting pupils, a
bulging anterior fontanelle and apneic episodes. There was no history of
bleeding diathesis, evidence of overt bleeds or external evidence of
injury, The child was intubated and ventilated, anti edema measures
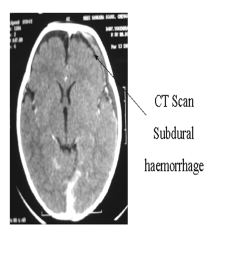
initiated and a head CT performed, The CT revealed a thin left subdural
hematoma with cerebral edema (Fig. 1). His full blood count
including platelet count was normal. His coagulation profile, renal and
liver function tests were within normal limits. A lumbar puncture was
withheld in view of features of elevated intracranial pressure. Other
investigations were non contributory. A neurosurgical consult was
obtained and a conservative approach planned as there was no mass effect
on CT scan.
 |
|
Fig. 1. CT brain revealing subdural hematoma. |
The initial provisional diagnosis was intracranial
infection and antibiotics were initiated in addition to anticonvulsants.
A fundal examination, however, gave an entirely new dimension to the
diagnosis. Both fundi revealed extensive retinal bleeds.
Armed with this knowledge, the parents were directly
and tactfully questioned regarding the possibility of the child having
been vigorously shaken, They admitted that an elder sibling aged 5 years
used to play frequently with his infant brother and at times had been
observed to have shaken him violently and vigorously. The history of
shaking, presence of intracranial and retinal bleed and no coagulopathy
allowed a firm diagnosis of shaken baby syndrome to be made. A CSF
examination after 48 hours was completely normal and antibiotics were
discontinued.
With supportive management, seizures were controlled,
mental status improved and episodes of posturing subsided. The tense
anterior fontanelle become flat and the child was extpbated on day 7.
Apart from opthal-mological abnormalities, the neurological examination
was normal. Vision was severely impaired with absent menace reflex and
bilaterally dilated sluggishly reacting pupils.
A detailed fundus examination including slit lamp
examination and flourescein angio-graphy was performed by an
opthalmologist which showed bilateral extensive preretinal, intraretinal
and subhyaloid hemorrhages.
The baby was discharged on day 11 and the parents
were adviced to strictly supervise with his elder brother. During a
follow up visit 6 weeks later his vision on the right eye had improved
and he was amblyopic on the left.
Discussion
Shaken baby syndrome should be suspected in all
children younger than one year of age who present with drowsiness, coma,
seizures or apnea. A combination of subdural hematomas, retinal
hemorrhages with minimal or no trauma and no coagulopatry is almost
pathognomonic of this syndrome. The findings are caused by shaking with
or without impact. Physical signs of violence are often absent and the
syndrome may easily be mistaken for a serious infection or seizure
disorder(1). The infant is held by the thorax and shaken. This causes a
repetitive acceleration deceleration trauma which leads to the typical
intracranial bleeding, eye injuries and paravertebral rib fractures.
Many cases are fatal or lead to seizures and neurological disability
including blindness. Cerebral palsy, mental retardation or epilepsy may
occur in about 60% of the children(1).
This syndrome was first described in 1974 by
pediatric radiologist John Caffey, who coined the term ‘infantile
whiplash shaking syndrome’ to describe the constellation of clinical
findings in infants with intracranial and intraocular hemorrhage in the
absence of external trauma to the head or fracture of the clavaria(3).
These shaking injuries were thought to be caused by the easily torn
bridging veins of infants head. The infants head and blood vessels are
particularly vulnerable to shaking and whiplash because of the
relatively large head and weak neck muscles of the child, the abundance
of unmyelinated brain tissue which permits excessive stretching of the
brain and vessels, and the increased pliability of the skull as compared
to the rigidly fixed internal soft tissue structures such as falx
cerebri(4).
In contrast to the "Battered Baby Syndrome" all the
findings in whiplash shaken baby syndrome of infants are subtle and
demand awareness, an index of suspicion and a fundus.
Intraocular haemorrhages can range from minimal to
severe. Therefore in a child under 3 years of age, the presence of
extensive bilateral retinal hemorrhages raises a very strong possibility
of SBS, which must be investigated(5).
Ophthalmic examination of children with suspected SBS
is important for prognostic as well as diagnostic purposes. Diffuse
fundic bleeds, vitreous hemorrhage or large subhya-loid haemorrhages are
usually associated with worse visual outcome(6). Non reactive pupils and
midline shifts of the brain structure correlates highly with mortality
and more severe neurologic injury. Many are fatal. Of the survivors,
upto 60% may have neuro-logical sequalae which include seziures,
cerebral palsy and blindness.
There is a spectrum of the consequences of SBS and
less severe cases may not be brought to the attention of medical
professionals. A victim of sublethal shaking may have a history of poor
feeding, vomiting, lethargy and or irritability occurring for days or
week. Signs of SBS may vary from mild and non specific to severe and
immediately identifiable clini-cally as head trauma. In the most severe
cases which usually result in death or severe neurologic consequences
the child usually becomes immediately unconscious and suffers rapidly
escalating life threatening CNS dysfunction(1).
Acknowledgement
We acknowledge the contribution of Dr. Janakiraman
Senior Consultant, Opthal-mology for ophthalmic examination and slit
lamp eye pictures.
Contributors: IJ and DG were responsible for
collecting the clinical data and literature search. All authors drafted
the manuscript. SR critically reviewed the manuscript. SR will act as
the guarantor of the paper.
Funding: None.
Competing interest: None stated.
