The clinical manifestations of VACTERL association
include vertebral anomalies, anal atresia, congenital heart disease,
tracheoesophageal fistula, renal dysplasia and limb abnormalities(1).
Prune belly syndrome is the triad of deficiency of abdominal muscles,
dilatation of urinary tract and crypt-orchidism(2). The association of
these two syndromes in a child has been reported probably once in
indexed literature(3). We report a case of VACTERL association who also
had all the features of prune belly syndrome and discuss the possibility
of a common etiology.
Case Report
A small-for-gestational age male neonate was born
vaginally at 37 weeks of gestation to a 20-year-old primigravida mother
and a 26 year old father. The family history was unremarkable and the
couples were non-consanguineous. The mother had no antenatal check up.
There was no obvious antenatal teratogen exposure, fever, rash or any
drug intake. There was no polyhydramnios or oligohydramnios and the
placenta was normal. The neonate had Apgar scores of 8, 9, 9 at 1, 5 and
10 minutes, respectively and a birth weight of 2.3 kg. The length of the
baby was 48 cm with an upper to lower segment ratio of 1.67: 1, chest
circumference of 28.5 cm and head circumference of 34 cm.
Multiple malformations were recognized at birth. The
anomalies identified on physical examination included esophageal atresia
with tracheo-esophageal fistula, anal atresia, a short and malformed
right upper limb with valgus deformity, absent right thumb and
rudimentary left thumb. The abdomen was distended with lax abdominal
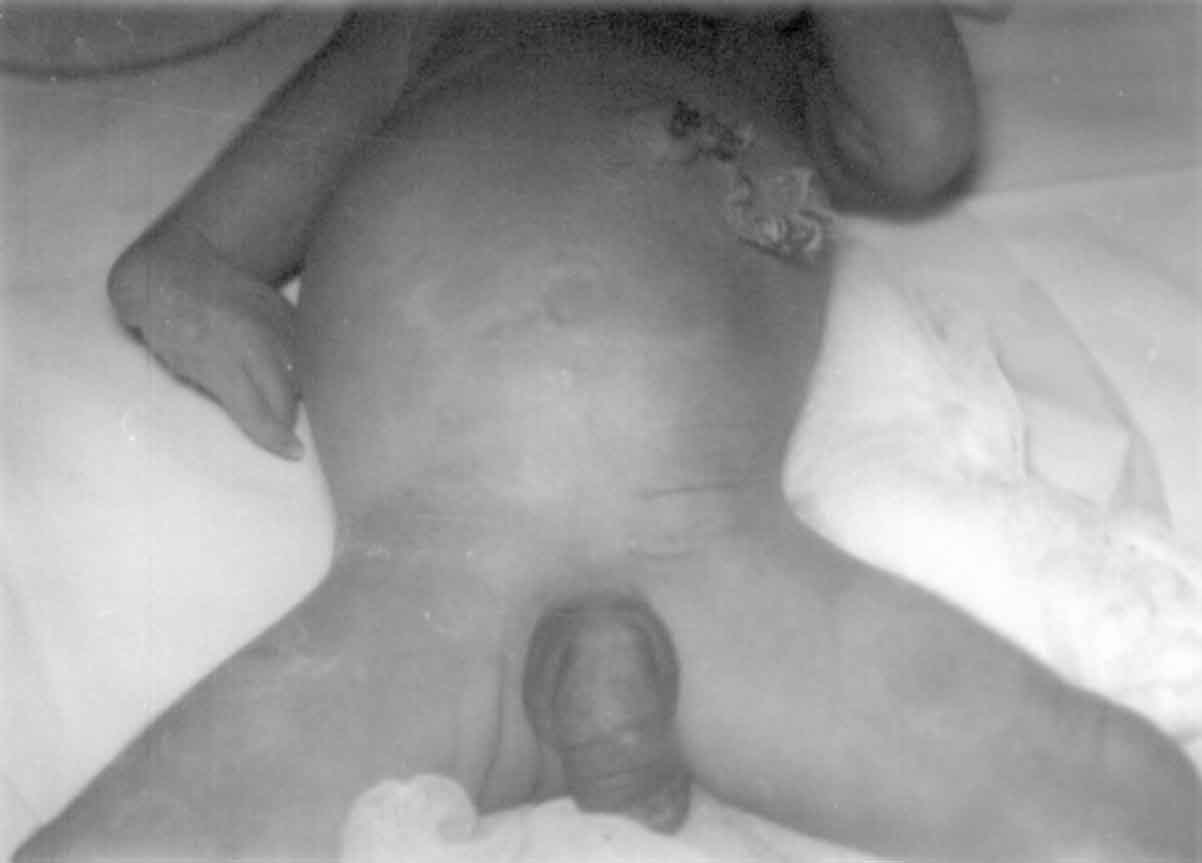
wall, a high placed umbilicus and single umbilical artery. The phallus
was large (megalopenis) with bilateral cryptorchidism (Fig. 1).
Urinary bladder was palpable and the overlying skin of the penis had
rugosities. There was a corneal opacity in left eye. Cardiovascular
system examination revealed a pansystolic murmur.
 |
|
Fig. 1. Prune Belly with high placed
umbilicus, large phallus, bilateral cryptorchidism and deformed
right upper limb. |
X-ray of chest showed coiling of the nasogastric
tube in dilated upper esophageal pouch with presence of gas in stomach
suggesting a diagnosis of esophageal atresia with tracheo-esophageal
fistula. Skiagrams of upper limbs showed absent radius and short ulna on
right side with absent first metacarpal in both hands. X-ray of
the lumbosacral spine showed fusion of L4-L5 vertebra. Ultrasonography
of the abdomen revealed a normal right kidney with non-visualization of
left kidney. Bladder was enlarged and thick walled with rest of the
viscera being normal.
On the basis of above anomalies, a diagnosis of
VACTERL association with Prune-Belly syndrome was made. The child had
severe respiratory distress since birth and was oxygen dependent. In
view of multiple major malformations, parents did not agree for a
surgical intervention and the child died on 3rd day of life. Autopsy
findings revealed bilateral intra-abdominal testes, which were found
normal for age on histopathological examination. Additional anomalies
found in autopsy were pulmonary hypoplasia, hypoplastic abdominal
musculature, bladder diverticula and megalourethra. The right kidney
showed glomerular cysts, a sign of early obstruction. In place of left
kidney, a tiny cystic structure was identified which on microscopy was
confirmed to be a cystic dysplastic kidney. Fusion of L4-L5 vertebrae
was also detected. The heart was normal except for the presence of a
patent ductus arteriosus.
Discussion
Our patient had vertebral body defects, anal atresia,
single umbilical artery, esophageal atresia with tracheo-esophageal
fistula, dysplastic kidney and radial defects; all classical features of
a full spectrum VACTERL association(4). The patient also had hypoplastic
abdominal wall musculature and urinary tract abnormalities suggesting
the additional diagnosis of a complete Prune Belly syndrome. The
complete form of Prune Belly syndrome consists of an abdominal wall
deficient in muscular tissue, dilated urinary tract, and bilateral
cryptorchidism and thus seen only in males(5).
Urogenital anomalies like unilateral or bilateral
cryptorchidism, hypospadius and micropenis in males and ambiguous
genitalia and bladder exostrophy in females have been frequently
described in VACTERL association(4,6). In the largest such series of 286
patients, 81 (28%) had severe genital defects(7). Abdominal wall
abnormalities like omphalocele and gastroschisis are also occasionally
reported(7) but concurrence of a full-fledged Prune-Belly syndrome is
extremely rare. Lukusa, et al.(8) described incomplete Prune
Belly anomaly in a female child with additional features of the VACTERL
association. Ozturk, et al.(3) for the first time reported
concordance of complete Prune Belly syndrome and VACTERL association in
a premature male child. Both the above cases did not have esophageal
atresia or tracheo-esophageal fistula. Full spectrum of VACTERL (all six
components) with a complete Prune Belly syndrome in our case reflects a
severe disruption of both cranial and caudal mesoderm.
Associations are derivatives of causally nonspecific
disruptive events acting on the developmental field which could be the
entire embryo during first four weeks of life(9). This pattern of
malformation generally has a sporadic occurrence in an otherwise normal
family. A disruption in differentiating meso-derm in first 4-5 weeks has
been suggested to be the basis for such a non-random association(7).
Other defects of mesodermal origin such as neural tube defects,
orofacial clefts, bladder extrophy and diaphragmatic defects are
occasionally seen in cases with VACTERL association. The overlapping of
defects of VACTERL association with CHARGE association and Goldenhar’s
syndrome have also been described(4). This overlap implies an etiologic
commonality which has been described as the axial mesodermal dysplasia
spectrum(10).
Early disturbance of mesodermal development in both
the abdominal wall and the urinary tract has also been suggested to be
responsible for Prune Belly syndrome(11). The timing of the insult
appears to be around third week of gestation which would account for all
three parts of the triad. Presence of single umbilical artery also
suggests the insult around the fourth week of intrauterine life(12). As
both VACTERL association and Prune-Belly syndrome have a common etiology
of a defect in the differentiating mesoderm in early first trimester, we
believe that concurrence of these two syndromes is another addition to
the axial mesodermal dysplasia spectrum.
Contributors: DS and SS were involved in patient
management, review of literature and drafting of the manuscript. DS
shall act as the guarantor. MMAF supervised the patient management and
critically reviewed the manuscript. KM conducted the autopsy and also
helped in drafting of manuscript.
Funding: None.
Competing interests: None stated.
