An 11-year-old boy presented with recurrent, self-healing, asymptomatic
eruptions involving trunk, over the last three years. The eruptions used
to start as small red papules, progressing centrifugally to form annular
plaques with a central clearing. No systemic features or mucosal lesions
were present. Physical examination revealed multiple erythematous
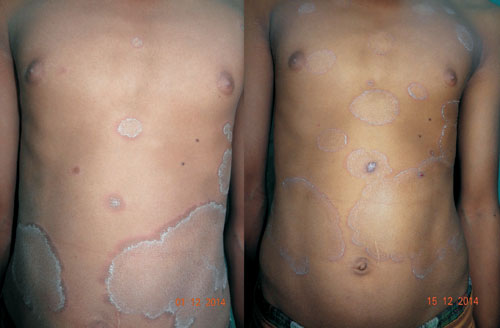
annular and polycyclic plaques, with trailing scaling at their inner
margins (Fig. 1).
The lesions were present exclusively on trunk; rest of the
muco-cutaneous examination was non-contributory. There was no
lymphadenopathy. KOH mount of scales did not reveal any fungal hyphae.
Blood investigations were non-contributory. Histopathology from the
erythematous margin showed mild hyperkeratosis, focal parakeratosis, and
perivascular lymphocytic infiltrate in the superficial as well as deep
dermis. The patient was diagnosed with erythema annulare centrifugum
(EAC).
(a)
(b) |
|
Fig. 1 Annular erythematous plaques
with trailing scales on trunk; on presentation (a), and after 2
weeks (b).
|
EAC is one of the figurate or gyrate erythemas,
others being erythema marginatum (transiently seen in acute rheumatic
fever), erythema migrans (rash of localized Lyme disease caused by
Borrelia burgdorferi) and erythema gyratum repens (usually
associated with visceral malignancy, pulmonary tuberculosis, lupus
erythematosus and azathioprine). EAC presents as asymptomatic annular,
arcuate, circinate, or polycyclic erythematous plaques with indurated
margin and a trailing scale noted on the inner aspect of the advancing
edge. Rapid progression is typically seen. The condition is recurrent
and the course may last 4-6 weeks to many years. It has been documented
in association with infections, drugs (Chloroquine, Hydroxychloroquine,
Piroxicam, salicylates, Amitrip-tyline, Hydrochlorothiazide etc),
pregnancy, and malignancy. The differential diagnoses include tinea
corporis (itchy, papules/ pustules at the margin and fungal hyphae on
KOH mount), subacute cutaneous lupus erythematosus, and other figurate
erythemas. Topical steroids usually cause resolution of the lesions of
EAC, but they do not prevent new lesions or recurrence. A search for,
and treatment of the underlying disorder is warrented, but an exhaustive
workup for occult malignancy for EAC alone is not recommended.

